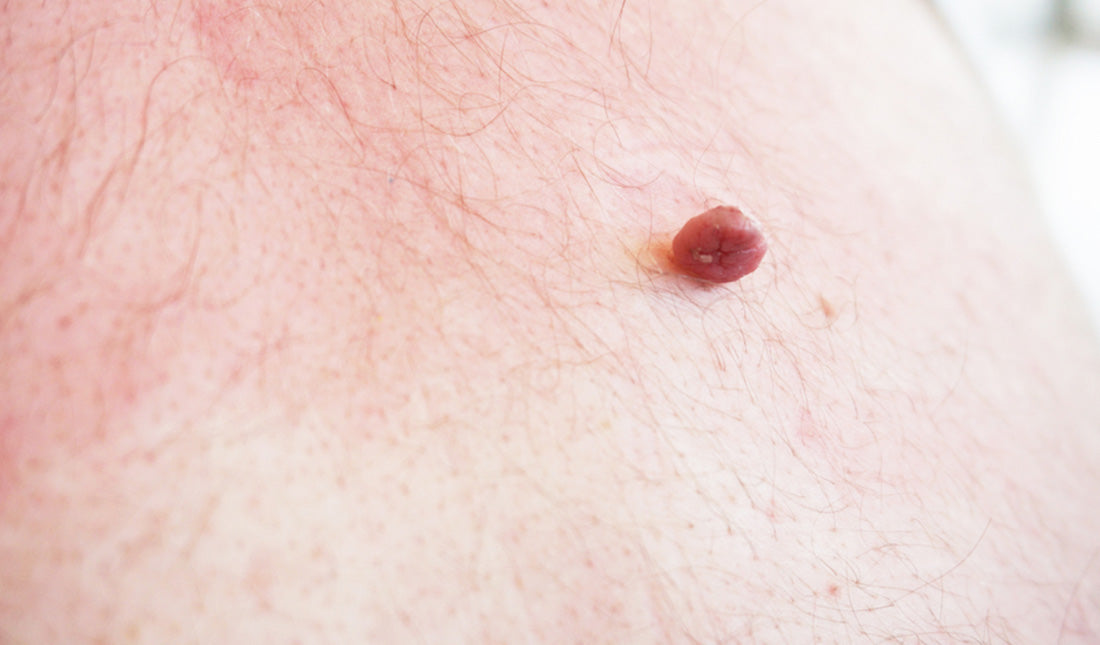
Tired of dealing with your skin tags? Although these small, fleshy pieces of skin are usually harmless, they can be incredibly annoying to deal with on an everyday basis.
Some people remove their skin tags because they keep catching on their clothing. Others choose to remove them strictly for aesthetic reasons.
No matter which camp you’re in, there are both right and wrong ways to go about removing your skin tags. If you want to know how to get rid of skin tags safely, you’ve come to the right place.
Here are three things you need to know on how to get rid of skin tags safely:
- Although skin tags are usually benign, many people find them irritating and don’t like the way they look
- Skin tags are often considered a cosmetic procedure and may not be covered by insurance
- It’s strongly recommended that you avoid attempting skin tag removal methods at home
What Causes Skin Tags?
Skin tags, also known as acrochordons and papillomas, are a benign skin condition that appears in the form of small, fleshy pieces of skin. Though scientists still don’t know much about skin tags, there are certain medical conditions and risk factors associated with their formation.
Insulin resistance, which is associated with prediabetes, may increase the chance of developing skin tags. In a 2010 study published in Anais Brasileiros de Dermatologia, researchers found a compelling link between the skin tags and insulin resistance (see claim: “The presence of multiple skin tags was strongly associated with insulin resistance irrespective of other risk factors.”)
Another theory is that skin tags are genetic. According to a 2019 study in Clinical, Cosmetic and Investigational Dermatology, certain genotypes are strongly associated with the development of skin tags (see claim: “…19 and rs6214 gene polymorphisms may contribute to a predisposition of STs in Egyptian patients.”)
Again, skin tags are usually harmless. However, their unattractive appearance and annoying tendency to catch on clothing lead many to consider options for skin tag removal.

The Problem with At-Home Skin Tag Removal
Thinking about taking a DIY approach to skin tag removal? Maybe it’s because you can’t be bothered to schedule a visit to the doctor. Maybe you don’t want to foot the bill for cosmetic skin tag removal.
Either way, we totally get it. That being said, many of the at-home skin tag removal methods are ineffective at best and dangerous at worst.
For example, one method of at-home skin tag removal involves applying Salicylic Acid to the problematic area. Sure, the Salicylic Acid in your acne cream is effective at eliminating pimples, but it’s NOT recommended for using on skin tags. When used incorrectly, Salicylic Acid can potentially lead to skin damage and scarring.
Another popular method that is equally as dangerous is using a piece of dental floss to strangulate the skin tag in the hopes that it will simply fall off. This method, along with snipping off the remaining skin, can leave skin sore and inflamed.
It can also increase your risk for infection. In many instances, people who attempt these methods end up at the hospital anyway due to the skin complications.

3 Safe and Effective Methods for Removing Skin Tags
The best way to remove your skin tags is by seeing a doctor—full stop. He or she will remove your skin tag using a safe and effective method.
Your doctor will also make sure that what you’re dealing with is actually a skin tag and not something else. As it turns out, many people confuse their skin tags for moles. Since moles have the potential to develop into skin cancer, it’s important to have suspicious lesions looked at by your dermatologist so they can be diagnosed properly.
Make sense? Good. When you visit your doctor, here are the three safe methods they might recommend to get rid of your skin tags:
Surgical Excision
If your skin tags are in a sensitive area such as the eyes, groin or anus, your doctor may choose to snip them off using a small pair of sterile scissors. He or she will numb the area before cutting through the “stalk” that connects the skin tag to the base.
The actual snipping takes seconds to do. Your doctor may follow up the cut with a cauterization technique (burning the base of the skin) to create a scab, which will help prevent infection and regrowth of the skin tag.
Cryotherapy
When doctors talk about “freezing off” your skin tag, they’re referring to cryotherapy. This technique involves liquid nitrogen application, which causes damage to the skin tag via intracellular ice formation.
Though it might sound cool, cryotherapy can have some unwanted side effects. It’s typically not used in sensitive areas because liquid nitrogen can cause skin irritation, headaches and hypopigmentation, among other symptoms.
Cauterization
The last option is cauterization, which involves burning off the skin tag by using heat from electricity. Your doctor will likely give you anesthetic beforehand, especially if the skin tag is on the larger side.
The benefits of cauterization for skin tags are vast. It’s fast, effective and leaves a scab that reduces the risk of infection and regrowth. It also stops the bleeding immediately, so you can go about your day without worrying about bleeding on your clothes.
Final Thoughts
Unfortunately, many skin tags are considered a cosmetic procedure and, thus, aren’t covered by insurance. This leads many to seek out dangerous, at-home methods for removing skin tags.
Before you turn to riskier removal methods, be sure to talk with your doctor about any irritating symptoms of your skin tag (itchiness, pain, etc.). This can potentially help build your case for getting your skin tag removal covered by your insurance.
References
Tamega, Andréia de Almeida, et al. “[Association between skin tags and insulin resistance].” Anais Brasileiros De Dermatologia, vol. 85, no. 1, Feb. 2010, pp. 25–31. PubMed.
Farag, Azza Gaber Antar, et al. “Role of Insulin-like Growth Factor-1 in Skin Tags: A Clinical, Genetic and Immunohistochemical Study in a Sample of Egyptian Patients.” Clinical, Cosmetic and Investigational Dermatology, vol. 12, 2019, pp. 255–66. PubMed.